INTRODUCTION
With more than 2 billion people (roughly 30% of the world population) being considered overweight or obese [1], excess body weight is considered one of the leading health problems in the 21st century [2]. The association between excess body weight and increased risk for cardiovascular and metabolic disease risk along with orthopedic problems, impaired pulmonary function, depressive symptoms and overall quality of life has been well documented [3,4]. In addition to the impact on individual health, weight-related health problems put a significant burden on the health care system as they have been estimated to make up 10% of all healthcare expenditures [5]. Particularly obesity has been associated with decreased productivity, increased number of doctor’s visits and hospital stays [6,7], resulting in 36% higher costs in both inpatient and outpatient spending along with 77% higher costs for medication compared to normal weight individuals [8].
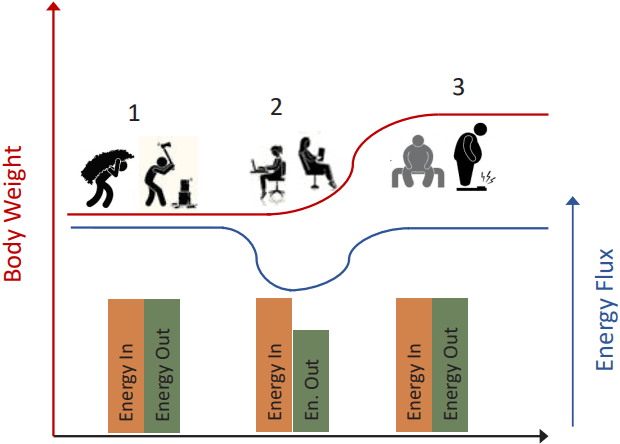
The rising prevalence of obesity [1], despite considerable efforts, also reflects the limited understanding of the complex interaction of cultural, psychosocial, biochemical, metabolic and genetic factors contributing to the regulation of energy balance. Based on the laws of thermodynamics energy intake (EI) and energy expenditure (EE) need to match over time in order to maintain body weight. Such a simple opposition of EI and EE, however, ignores the complex interaction of physiological and environmental constraints within the concept of energy balance [9]. Body weight should not be viewed as a simple outcome based on the interaction of EI and EE but rather as an additional component within the energy balance system (Figure 1). Alterations in body composition, for example, are associated with changes in resting metabolic rate and energy requirements for various movements [10]. Further, body composition has been suggested to affect dietary intake [11]. An additional problem in the accurate matching of EI and EE is that EI occurs in episodical events while EE is a continuous process. Accordingly, the human body is almost constantly in energy imbalance – an energy surplus following a meal and an energy deficit during various activities without any food consumption, including sleep [12]. There is also considerable variability in daily EI and EE with little association between EI and EE on a daily basis. Even in people who are considered to be in energy balance (i.e. maintenance of body weight), it has been shown that EE and EI do not match on a daily basis [12-14]. Small differences between EI and EE, however, can have significant effects on body weight in the longterm [15]. In fact a commonly observed annual weight gain between 0.5 and 1 kg per year has been associated with an energy surplus of only 50 to 100 kcal/day [16]. These small differences, however, may be difficult to detect by various physiological systems and it has been argued that macronutrient intake rather than total EI are regulated [17]. Social constraints potentially affect energy balance as well and may override physiological processes as people tend to put on weight in a non-linear fashion with a more pronounced weight gain during the weekend compared to weekdays as well as during certain times of the year (i.e. winter holiday season) [18-20]. Accordingly, data from pharmacological weight loss trials lead to question a body weight control system [21].
The Role of Energy Flux in Weight Management
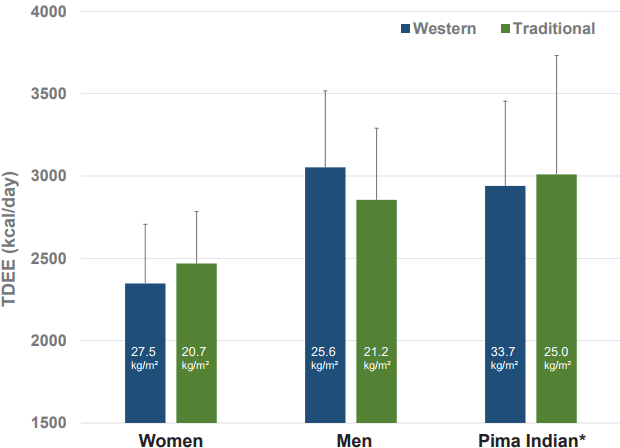
Even though an imbalance between EI and EE is ultimately responsible for weight change, the rate of EI and EE along with alterations in body weight, which is also referred to as energy flux [22], has been suggested to play an important role in weight management as well. Theoretically, energy balance can be achieved at various levels of energy flux (i.e. low EE matched by low EI or high EE with high EI) but a higher energy flux has generally been associated with a better matching of EI and EE [23,24]. These studies attributed a higher energy flux to high levels of physical activity (PA). Alterations in body weight, however, affect energy expenditure and accordingly energy flux as well [10]. Using doubly labelled water it has been shown that total daily energy expenditure (TDEE) does not differ between populations pursuing a traditional lifestyle, characterized by high physical activity and those living a typical western lifestyle, characterized by predominantly sedentary habits [25,26] (Figure 2). There was also no difference in TDEE between populations living in low, middle or highly, developed countries [27], indicating a similar energy flux. A sedentary lifestyle, generally observed in industrialized countries, however, was associated with significantly higher body weight [25-27].
Similarly, there was a comparable EI between men with sedentary occupations (i.e. clerks) and those engaging in heavy work (i.e. blacksmiths, cutters, carriers), despite considerable differences in PA and body weight [28]. A recent study also did not show any change in average EE or EI over a period of 2 years in participants who experienced a significant weight change [29]. While these participants certainly experienced alterations in EE and EI in order to induce weight change, these alterations may have been small in nature and, therefore, difficult to detect. There were, however, significant behavioral changes with an increase in PA in participants who lost weight and a decrease in PA in those who gained weight, allowing participants to maintain their EE and EI despite alterations in body weight. Accordingly it may be speculated that energy flux, rather than energy balance, is a regulated entity and that human beings use different strategies to achieve a certain energy flux; either sufficient PA or increased body weight.
The importance of a high energy flux in order to maintain energy balance may be a result of the development of human physiology under circumstances of high PA demands and accordingly high energy flux [30]. In fact, participation in PA has been considered a biologically normal condition in pre-industrial eras [31,32]. At the same time, there was a limited supply of food in the past, which emphasized the need to minimize energy output and potentially facilitated the development of a homeostatically controlled TDEE in order to ensure survival [28]. As a result, an upper threshold for TDEE and energy flux would have been determined based on the interaction of food availability and PA (required to obtain food and ensure survival). Data from animal and human studies in various environments support the theory of a physiologically constrained energy flux [33]. For example, there were no differences in EE or EI between monozygotic twins who differed in PA levels and body composition [34,35]. Similarly, there was no difference in TDEE between members of an Indian tribe living a predominantly sedentary lifestyle with accompanied increased body weight in a U.S. reservation and those following a traditional lifestyle, characterized by high PA and lower body weight in Mexico [26]. It has also been shown that EI does not change in response to long-term alterations in PA while overeating has not been associated with alterations in PA [36]. An insecure food supply may have contributed to a predisposition of overeating and storage of excess calories in the form of fat during times when excess food was available in order to prepare for times with sparse food availability [37]. In the modern environment foods, however, are readily and constantly available while high amounts of PA are no longer required, resulting in a mismatch between physiology and environment as human beings have developed biological adaptations for hunger but not for overconsumption [38,39]. Given this situation, increased body weight can be viewed as a normal and predictable biological adaptation to a sedentary lifestyle in order to achieve a homeostatic state at a physiologically predetermined energy flux [40] (Figure 3).
Practical Implications
Given the importance of PA in weight management and the fact that the majority of people in industrialized countries have sedentary occupations, a critical question would be how to incorporate a sufficient level of PA in our daily lives. Even though active travel has been promoted as viable option, the contribution of active travel to TDEE has been considered negligible [51] and Ohkawara et al. argued that the general population is unlikely to achieve the necessary volume of locomotor activities to affect TDEE [52]. While activities such as walking have beneficial effects on chronic disease risk these activities had limited effects on energy expenditure and body weight [53]. In order to affect body weight and body composition, activities of higher intensities appear to be necessary [54-57], which most likely warrant a more structured approach, such as exercise.
Traditional aerobic exercise interventions, however, have been of limited success particularly in overweight and obese participants [58]. This has, in part, been attributed to compensatory reductions in habitual PA, which would have minimized exercise-induced alterations in TDEE [36,59]. Resistance exercise, on the other hand, has been associated with increased functional capacity that allows participants to engage in additional activities outside the exercise intervention [60-62]. Resistance exercise has also been associated with an increase in fat oxidation [63], which could have positive effects on body composition. Another approach, particularly in children, could be a focus on motor development as increased motor competence facilitates the engagement in various physical activities [64]. Overall, intervention strategies should focus on facilitating participation in various activities, including habitual PA as this may enhance the chances that participants continue with an activity lifestyle beyond the intervention period and, therefore, provide more sustainable results.
SUMMARY
Given the limited success in addressing the obesity epidemic, the consideration of a stable energy flux could provide a valuable framework for the development of strategies addressing the obesity epidemic. If energy flux is considered a regulated entity, its regulation must occur via complex interactions among key components of energy balance with changes in body weight and PA representing critical opposite forces in the regulation of energy flux. In such a scenario weight gain would be simply a means to maintain energy flux at low PA levels. It remains to be determined, however, whether alterations in PA precede changes in body weight or whether it is a response to weight gain or weight loss. A hypothesized individually predetermined energy flux also takes a more encompassing approach towards the regulation of body weight including a gene-environment interaction [15]. An inter-individual variability in energy flux could help to explain the differences in body weight between people living in a similar environment as not everybody exposed to an obesogenic environment experiences excess weight gain. It can be speculated that people who are predisposed to a higher energy flux may actually be at increased risk for excess body weight in the modern environment as they can easily achieve a high EI while high PA requires considerable conscious efforts. These people may also have developed more efficient strategies in storing excess calories. Those who have a lower predetermined energy flux, on the other hand, may consume less calories and/or are less prone to store excess calories even in the current environment and, therefore, could maintain a healthy body weight with lower PA.
Considering energy flux as a regulated entity further explains why people who are currently obese would not be able to maintain weight loss by dietary restriction alone. Weight loss, due to dietary restriction ultimately results in a lower energy flux, which would trigger compensatory effects, such as an increase in appetite followed by an increase in body weight; a situation that usually occurs with this type of weight loss intervention [65,66]. A reduced EI in order to loose weight with an accompanying increase in PA, on the other hand, would allow individuals to maintain a lower body weight when EI returns to initial levels resulting in an energy flux level that is not significantly different from that seen prior to weight loss. Even though more research is needed to clarify the role of energy flux and potential physiological constraints associated with the regulation of energy flux it emphasizes the critical role of PA in long-term weight management.